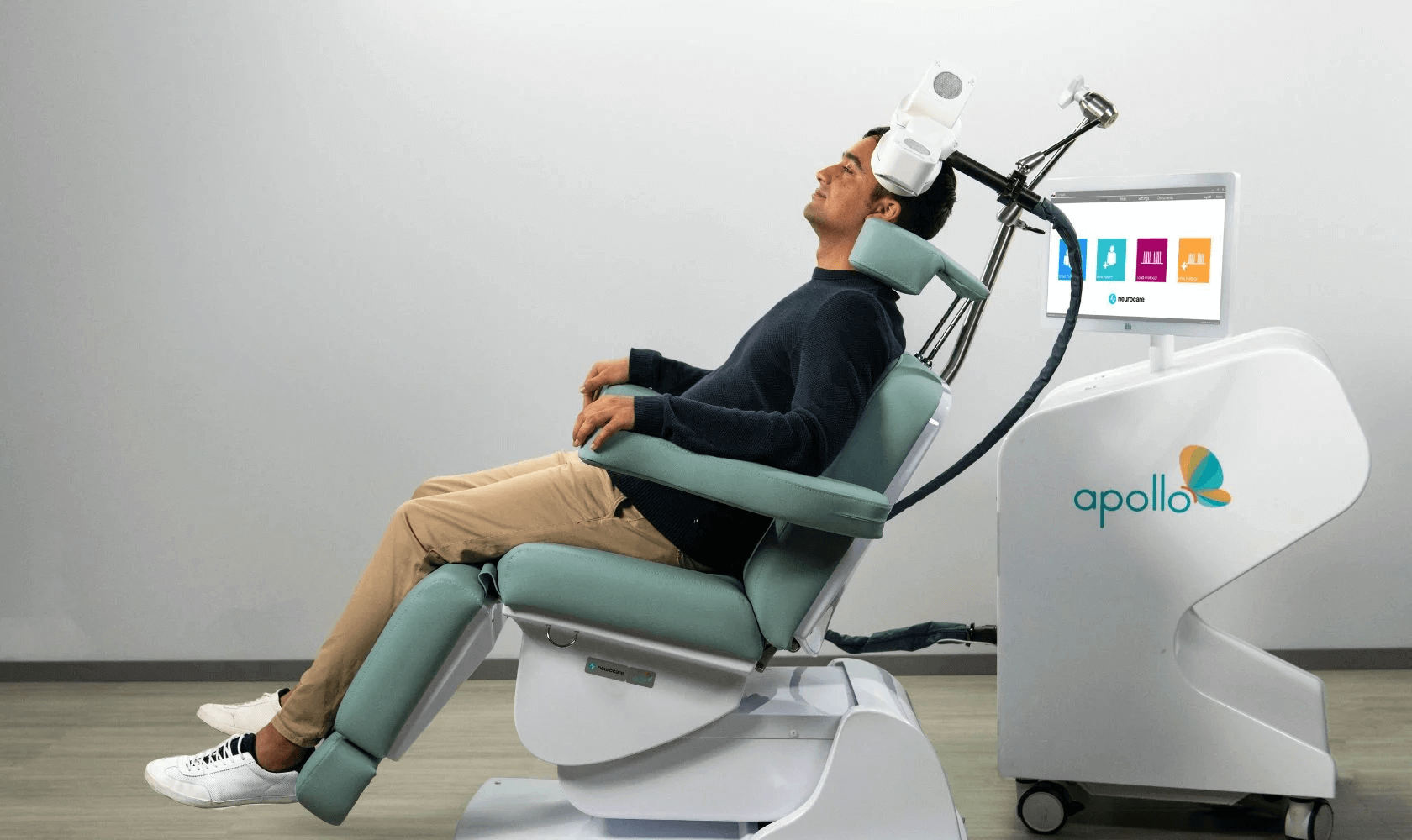
Transcranial Magnetic Stimulation (TMS) is a non-invasive brain treatment unlike any other. With a coil on the scalp, magnetic pulses are sent into parts of the brain that regulate mood. It’s an outpatient treatment, nonsurgical and with no anesthesia, that is generally used for treatment-resistant depression (TRD).
The FDA approved TMS for depression in 2008, as well as OCD (2018) and smoking cessation. The U.K. has similar guidance through NICE.
Table of Contents
You may be wondering how TMS works.
A TMS device generates magnetic pulses to stimulate nerve cells in specific areas of the brain, usually in the left dorsolateral prefrontal cortex. Once a certain number of treatments is reached, these magnetic pulses will “reset” the circuits in the brain that control mood and motivational functions.
Depending on the frequency of the magnetic pulses generated by the device, there are several different responses to brain activity. There are even accelerated options in which the TMS system can be programmed to deliver a variety of short TMS therapy sessions daily, allowing for results to be achieved as quickly as possible.
Types of TMS
- rTMS: This is a standard therapy, delivering 20-30 sessions over 4-6 weeks
- Deep TMS (dTMS): This method uses specially calibrated coils (H-coils) and can stimulate deeper regions. FDA approved to treat depression and smoking.
- Accelerated TMS: This option allows several treatments to occur in a day, and it is often possible to condense all the treatments into just one week.
Conditions Treated
Approved uses:
- Major Depressive Disorder (especially TRD)
- OCD
- Smoking cessation
Research areas include PTSD, bipolar depression, migraine, chronic pain, and cognitive decline.
Who’s Eligible?
TMS may be appropriate if:
- You have tried and not gotten better with medication or therapy.
- You can commit to daily visits.
Not appropriate for:
* People with metal implants in their head (such as an aneurysm clip).
* People with uncontrolled seizure disorders.
How a Course Works
- Mapping: The clinician identifies the applicable brain location using test pulses.
- Sessions: 5 days/week for 4 – 6 weeks (20 – 40 minutes long).
- Check-ins: weekly progress checks.
- Boosters: optional maintenance sessions.
Effectiveness
The studies done to date have shown that TMS outperformed sham treatments for TRD. Response and remission rates are promising, and often the effects last for many months, especially with the boosting sessions.
Safety & Side Effects
Common: Scalp discomfort, headache, facial twitches, or lightheadedness (typically mild).
Rare: Seizures (very rare with proper screening).
Precautions: Ear protection is used because it can be loud.
TMS vs Medication vs ECT
- Medication: widely available but can include systemic side effects.
- TMS: non-invasive, outpatient, does not use anesthesia, and almost no cognitive side effects.
- ECT: very effective but requires anesthesia and can raise risk of memory issue.
What You Need to Know Before Your First Session
* Provide full medical and medication history.
* Avoid metal or metallic accessories near the coil.
* Eat and stay self-hydrated as you normally would.
* If you suspect you will want to have multiple daily appointments, plan ahead.
During and After the Session
There may be a sensation of tapping and a clicking sound that occurs. Most people will return to their regular activities immediately after. Headaches, if any, usually go away with time.
Pragmatics: Cost & Insurance
For most insurers, TMS is covered if and only if you have attempted treatment with standard therapies first. If you are going to self-pay, costs are very varied, and clinics may have packages or payment plans.
Myths versus Facts
- Myth: TMS is “shock therapy.”
- Fact: It uses magnets, not electrical shocks.
- Myth: TMS alters personality.
- Fact: It makes symptoms less severe without changing personality.
- Myth: TMS works instantaneously.
- Fact: Progress is slow, most often over the course of weeks.
Conclusion
Transcranial Magnetic Stimulation (TMS) is a safe, effective, and non-invasive option for those who have not been able to find relief with medication or therapy. As FDA approval continues, protocols continue to expand & safety data continue to be strengthened, TMS is likely to gain traction & become a more mainstream treatment not just for depression, but also for other applications.
If you’re considering TMS, now it’s the time to take the next step. Reach out to a qualified provider, inquire about the common questions on TMS, discuss if TMS could be a part of the recovery process, and find out what options are available to you.
Frequently Asked Questions (FAQ’s)
How long until I see results?
Typically, it can take around 2-4 weeks into treatment.
Can I drive after TMS?
Yes, there is no sedation involved.
What are the most common side effects?
Scalp discomfort and mild headaches.
Is it safe to have dental fillings or braces?
Yes, these are safe, but you must inform your provider of these presents.
How many sessions will I need?
In total, people typically might receive 20-30 sessions in around 4-6 weeks.
Is TMS the same as ECT?
No, ECT involves anesthesia and incites seizures; TMS does not.